-
Ebola virus disease has caused havoc in West Africa, with 11, 162 deaths and more than 27, 181 cases (as of May 31, 2015) being reported since the virus emerged in early 2014 in Guinea. The maximum number of cases has been reported in Sierra Leone (12, 827), while most of the reported deaths have occurred in Liberia (4, 806), according to the Center for Disease Control and Prevention (CDC; http://www.cdc.gov/). An increased number of cases in countries like Guinea, Sierra Leone, and Liberia has created an emergency medical situation. The disease spread from Guinea, and cases were initially observed in neighboring countries and in Nigeria, the most populous country in Africa. Local and international medical experts are working hard not only to limit the spread of infection but also to reduce misunderstanding and misinformation among the public, which causes additional problems.
Ebola virus was first identified in 1976 in Yambuku, Democratic Republic of Congo and in Nzara, South Sudan. The virus has an RNA genome and belongs to the Filoviridae family. It was given the name "Ebola" based on a river that runs through Congo. The filovirus family has fve species, of which one (Reston ebolavirus) does not cause disease in humans and four (Zaire ebolavirus, Bundibugyo ebolavirus, Taï Forest ebolavirus, and Sudan ebolavirus) are pathogenic to humans (Fauci, 2014). The strain that caused the current outbreak has 97% homology with Zaire ebolavirus (Baize et al., 2014). The viral strain is highly fatal (90%), and the current outbreak has shown a fatality rate of approximately 60% (CDC, 2014). Ebola virus is a zoonotic pathogen, and the current outbreak probably originated from an animal reservoir (most likely the fruit bat); however, this has yet to be confrmed (Fauci, 2014).
More than 20 outbreaks of the virus have been recorded (Table 1) since its first identification in 1976, causing approximately 1, 600 deaths before the recent outbreak (CDC, 2014). Most of the outbreaks occurred in remote and rural areas of Africa and, accordingly, were easy to manage, as a large population was not at risk. However, the current outbreak has spread to vast areas owing to a lack of disease awareness and education. In addition, the local health infrastructure is insuffcient to tackle the growing rate of infection. The general population, with the help of experts, can limit the spread of infection by sticking to standard hygiene and health practices and by sterilizing infected materials.

Table 1. Known cases and outbreaks of Ebola cirus disease
It is also possible for an asymptomatic patient to board a plane (or any other means of travel) and reach another country or countries owing to high global traffic; however, the chances of spread are still low because the virus is not airborne. The virus is not transmitted from infected to uninfected individuals by air or casual contact. To acquire the infection, one has to be exposed to infected body fluids like feces, blood, or vomit (Fauci, 2014). Almost all countries have made special arrangements at airports to stop the spread of infection.
It is very hard to recognize the signs of Ebola infection; the early symptoms are non-specific. The virus normally has an incubation period of 5–7 days; however, it can be as short as 2 days and as long as 21 days. It is possible to test for the virus by polymerase chain reaction before the onset of symptoms. The symptoms of the infection include fever, diarrhea, weakness, abdominal pain, headache, and vomiting. In some patients, a maculopapular rash also appears, and hemorrhagic complications occur in less than half of all patients; however, gross bleeding is relatively rare (Bwaka et al., 1999). When an individual becomes infected with the virus, it is necessary to take all public health measures including early isolation of the patient and infection control. There is also a need for aggressive supportive care to ensure patient survival and reduce death tolls.
There is no licensed therapy or treatment for Ebola virus disease. One therapy that is in development is a combination of humanized mouse antibodies called "ZMapp", which was initially used to treat non-human primates and has shown promising results. Later, the same drug was tested on two American healthcare professionals who were infected in Africa and brought to the USA for treatment. In both cases, the patients showed signs of clinical improvement that could be attributed to ZMapp (but additional studies are required to determine the effectiveness of the drug). According to Scientifc American, both patients are now fully recovered (Dina, 2014). This drug has been produced on a trial basis, and it will take time to scaleup the production of ZMapp. Other candidate drugs include an inhibitor of viral RNA polymerase and RNAibased nanoparticles targeting viral protein production. In addition, work on various candidate vaccines and their preclinical evaluation is in progress. One of the candidate vaccines developed at the National Institutes of Health (NIH; Bethesda, MD, USA) will soon enter into a phase 1 clinical trial, and human clinical testing for some of the other vaccines is expected to start by 2015. The drug favipiravir (Avigan), which was developed against influenza, could also be effective against Ebola and a similar response is expected theoretically, although it has not yet been used clinically (ABC News, 2014).
In the last 50 years, such deadly outbreaks have been rare in developed countries, which have suffcient resources to handle emergency medical situations that arise. Developed countries have an excellent capacity to isolate infected individuals and other suspected cases. In addition, health officials have the necessary training to meet such challenges and to trace and monitor contacts of the infected patients. Safety levels are well established in hospitals and research centers, which have appropriate protocols in place to handle patients, biohazard waste, and corpses. They also have the necessary biosafety equipment and the trust of the common public. However, this is not the scenario in developing countries, especially in African countries, which have a long history of conflicts and famine. In addition, most countries in the developing world are already facing challenges related to endemic diseases like malaria, tuberculosis, hepatitis, and HIV/AIDS. Due to violent conflicts, health infrastructures have been destroyed, and those that have not been destroyed do not have the capacity to handle outbreaks. Healthcare professionals do not have adequate training to meet these challenges, and the necessary protocols have not been established. There is also a defciency in biosafety measures and in the availability of personal protective equipment's (PPEs). If medical authorities and practitioners cannot find PPEs for themselves, they will be unable to provide to the common public. This creates additional panic (and attacks for PPEs on hospitals). Traditional practices and misunderstanding of information also complicate the situation, leading to mistrust in the public toward government policies and health officials. Furthermore, the public does not take warnings seriously. If an outbreak occurs, the porous borders with neighboring countries enable the rapid spread of infections. Such outbreaks in densely populated countries could be very serious because most developing countries do not have sufficient infrastructure; this would further destabilize their economies. Developed and developing countries should be prepared to cooperatively meet any such challenge.
The recent outbreak of influenza A (H1N1) resulted in 154, 000 cases and 842 deaths being reported in China in 2009. It had a huge economic impact, although the virus was much less virulent than the influenza A (H5N1) strain (Zhang and Wilson, 2012). Therefore, it is necessary to build the necessary infrastructure and train the appropriate personnel in developing countries to meet these emerging health-related issues and challenges.
Many developing countries lack a functional health care system, especially African countries. Such a system is not only important to monitor emergencies but also to develop an integrated response; otherwise, any epidemic can spread rapidly (as was observed in the case of Ebola) and pose huge problems worldwide. According to WHO reports, the basic health care system in most countries affected by Ebola is very fragile (http://www.who.int/healthsystems); substantial investments are needed to improve the infrastructure and bring reforms. This is not only important for African countries; in fact, most developing countries need additional investments to improve the healthcare sector. In addition, hospitals, especially emergency departments, are very crowded in most developing countries—an issue that needs immediate attention (Mehmood et al., 2012). Both developed and developing countries are facing grave problems related to communicable and non-communicable diseases; however, developing countries are more vulnerable and exposed due to demographic, geographic, and socio-economic factors. These factors result in poor healthcare and research facilities in most of the developing countries and this vulnerability further weakens the economy. The situation can be improved by focusing on developing and implementing effective preventive measures (Preedy and Watson, 2010; Ashraf and Ahmad, 2015).
The following are some recommendations to improve the healthcare situation in developing countries and to fight against infectious diseases.
1. It is necessary to improve the basic understanding of infectious diseases among the common public as well as suggest approaches to stop the spread of infections.
2. Basic hygiene and protective behavioral measures should be maintained in normal conditions and, especially, during emergencies. Most infections spread owing to lack of proper hygiene and protective measures (e.g., hand washing, disinfection, and safe burial practices).
3. There are fewer Biosafety Level 3 and 4 (BSL-3, 4) laboratories in developing countries than in developed countries; accordingly, it is necessary to establish more laboratories in developing countries or increase the number of regional laboratories. To date, there are only two BSL-4 laboratories in Africa compared to 13 operational BSL-4 laboratories in the United States. And three African countries have standard BSL-3 laboratories (Figure 1; http://fas.org/).
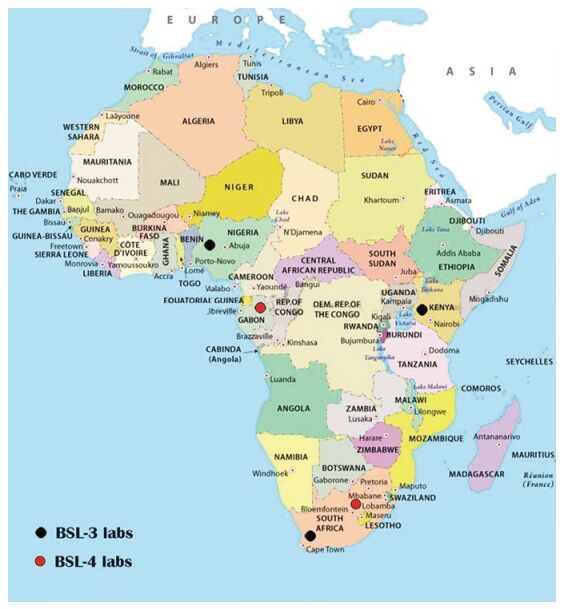
Figure 1. Standard biosafety level 3 and 4 laboratories in the African continent. Black circle: BSL-3 laboratory (In: Nigeria, Kenya, South Africa); red circle: BSL-4 laboratory (In: Gabon, South Africa).
4. It would be wise to establish an emergency response team or unit in each developing country, possessing all the necessary training and clear guidelines for tackling emergencies, which can act immediately after an outbreak in collaboration with national or regional BSL-4 laboratories. This will decrease the dependence on developed countries to tackle such problems.
5. There should be more training opportunities for scientists and clinicians related to biosafety and biosecurity in developing countries. Scientists and clinicians can be trained in developing or developed countries. Recently, the American Society for Microbiology arranged a series of biosafety training workshops for young scientists and clinicians in Pakistan in collaboration with the National Academy of Young Scientists (Pakistan); these workshops proved to be very helpful in improving the knowledge and understanding of standard microbiological practices. In addition, participants were introduced to and made familiar with personal protective equipment and their applications. Similar programs can be introduced in other developing countries to increase the number of skilled personnel.
6. Most hospitals in developing countries do not have specialized isolation units, making it diffcult to isolate infected patients. Arrangements should be made to establish isolation units in specialized hospitals along with the necessary infrastructure and protocols to monitor infected patients. All developed countries have specialized units for the isolation of infected patients.
7. Substantial funding should be allocated by governmental and non-governmental organizations to improve basic health care infrastructure in developing countries to ensure that emergency medical situations are tackled in the proper manner.
HTML
-
We acknowledge all the researchers and health care workers who contributed to stop the spread of Ebola infection. The authors declare that they have no conflict of interest. This article does not contain any studies with human or animals subjects performed by any of the authors.












 DownLoad:
DownLoad: