-
The epidemic in Russia was first recorded between 21st to 27th of September 2010 in South Sakhalin and cases were recorded in Kazakhstan three weeks later (October 16-22, 2010) in the north-east territories at the border of Siberia and Ural. The same as in Russia epidemic in Kazakhstan spread westward and southward.
The epidemic in Kazakhstan had moderate levels of intensity and differed from territory to territory as in Russia. In Astana and the north-east the epidemic intensity was higher in terms of duration (8-10 weeks) and morbidity level (7.8 -4.7 %) than in the south and south-west of Kazakhstan (4 weeks, morbidity 0.9% and 1.4%). Epidemic duration in Siberia and Ural (7.8 and 7.5 weeks) and morbidity level (10.2% and 9.6%) were higher than in the South and Privolzskiy federal regions (5.8 weeks and 5.7%). Morbidity levels in Russian regions was higher than in Kazakhstan because morbidity among city dwellers is normally higher than among country people.
In Kazakhstan the distribution of influenza and ARVI patients cases by age structure showed differences to the number of cases in Russia. The number of children's cases (age < 14) was more than in Russia 65, 0% and 52, 4% respectively.
Among infected > 65 aged people was slightly different in Kazakhstan and Russia and approximately equal (1.7% and 1.9%). Lethality from laboratory-confirmed influenza was 3.2% in Russia. Among people died in this epidemic in Russia people at ages 18-53 was 78.8%, and > 65 aged people -2.4%. Risk factor of lethal outcome from influenza was chronic pathology along side with late pregnancy.
Epidemiology in Kazakhstan resembled to Russian epidemic in terms of its abnormally early beginning (usually in December-January), expression of monoaetiology, spread of the epidemic into all territories and the identification of the first cases among the adult population. A higher percentage of hospitalized people and lethal outcome were registered in this epidemic. The similarity of the epidemiology of the outbreak in borderline territories of the two countries was investigated.
HTML
-
MHC data was used to determine cases of influenza and ARVI and the quantity of registered influenza cases and ARVI hospital patients with these diagnosis was recorded each week in October 2010 and classified into age groups of children aged 0 to 4 years old, 5-14 years old and adults aged 15 to 29 years old, 30-64 years old and > 65 years old for 2 cities (Astana and Almaty) and 14 oblasts. These data about were then used to characterize the epidemiological process induced by influenza and ARVI in RK.
Epidemiological control of influenza and ARVI in the Russian Federation is realized by the Federal Center of influenza and ARVI on the base of Research Institute of Influenza to Sain Petersburg and its 49 locations in major cities situated in different climatic and geographic regions [6]. The data from cities contain information about the number of registered influenza cases and ARVI for each week, hospital patients with these diagnosis and cases of death from influenza and ARVI all over the population and in groups of children aged 0 to 2 years old, 3-6 years old, 7-14 years old, adults aged 15 to 64 years old and older than 65 years old. Using these two datasets allowed us to compare the particular characteristics of the outbreaks in both countries during the 2009-2010 season.
-
Analysis of weekly influenza and ARVI morbidity in RK showed that influenza epidemic A(H1N1) had started in the 42nd week (October 16-22, 2009) in the territory of Karaganda oblast (Table 1). By week 43 week (October 23-29, 2009) an increase in morbidity was observed in Astana and in the territories of Pavlodar, Eastern Kazakhstan, and Northern Kazakhstan and Kostanay oblasts Morbidity for this week, as compared to previous, in Astana, Eastern Kazakhstan and Kostanay oblasts increased in 3, 2, and 1, 5 time, accordingly. And in Pavlodar and Northern Kazakhstan oblasts too exceeded the control levels of morbidity.

Table 1. Involving sequence and border of A(H1N1) 2009 epidemics in the Republic of Kazakhstan
In the 44th week (from the 30thOctober to the 5thNovember) an increase in morbidity was observed in the territories of Almaty, Akmola and Kyzylorda oblasts. In the 45th week (from the 6th to the 12th November 2009) the population of Atyrau, Southern Kazakhstan and Western Kazakhstan oblasts was involved in epidemic. In week 45 (from 13th till 19th of November) the Almaty city, Mangystau and Aktobe oblasts also recorded their first cases. The final territory included in the epidemic was Zhambul oblast.
By this point a peak in the number of cases was already registered in the territories which were involved in the earlier stages of the epidemic. In 46th week (from 30th to 5th November 2009) a peak was observed in Astana, a week later in Pavlodar and then in Karaganda oblast. The next three weeks (47-52 weeks) from November 20 till December 10, 2009 morbidity peaks were registered in Almaty and in all other oblasts. On average the morbidity peak throughout the country was for a week from 27th of November till 3rd of December. The peak started very soon in Astana and Almaty (2 weeks) as well as in Mangystau and Zhambyl oblasts; in Eastern Kazakhstan and Northern Kazakhstan oblasts the peak was not observed until 6 weeks after the first cases, on average the peak was observed in the 4thweek after the beginning of morbidity increase in these territories (Table 2). Influenza and ARVI morbidity during the epidemic peak on average was 822.1 with extremes of 311.2 (Southern Kazakhstan oblast) and 1542.2 (Astana) cases per 100 thousand people.

Table 2. Time of peaks in influenza and ARVI morbidity in 2009-2010 epidemic in Kazakhstan territories
Epidemic morbidity increase in the Republic of Kazakhstan was first observed among adults aged 15-29 and 30-64. Subsequently, cases in children were also recorded. An epidemic peak (maximum influenza morbidity and ARVI during a single week) among the young people (ages 15-29) was observed one week earlier than in other age-specific groups.
The epidemic in Kazakhstan lasted for 11 weeks (from the 16th October to the 31st December 2009. The duration of the epidemic in separate territories on average was 6.7 weeks with extremes of 4 weeks in the South (Mangystau and Zhambyl oblasts), 8 weeks (Karagandy, Northern Kazakhstan, Almaty, Eastern Kazahstan, Kyzylorda and Southern Kazakhstan oblasts) and 10 weeks (Astana) (Table 3).

Table 3. Duration of influenza and ARVI morbidity during the 2009-2010 A(H1N1) epidemic in the territories of Kazakhstan
The mean value of influenza and ARVI morbidity rates per 100, 000 for the entire population was 3326.3 among adults -1362.9 for children aged 0-14 years old was 7952.6. The highest morbidity level during this epidemic was registered in Astana with 7800.5 cases, children aged 0-14 -22837.0 and older than 15 -3236.5 per 100 thousand people. The lowest level of morbidity were registered in the Southern oblasts of Kazakhstan; for example, in Zhambyl oblast the population morbidity was 932.6 including population older than 15 -456.7 and children aged 0-14 -2137.5 cases per 100 thousand people.
Children aged 5-14 consisted the greater part of the influenza infected population. The percentage of infected children was 37.8% in the whole territory of Kazakhstan and varied throughout the territories from 28.9% in Kyzylorda oblast to 47.8% in Western Kazakhstan oblast (Table 4). Also, influenza and ARVI infections in children aged 0-4 was 27.2% nationally with fluctuations from 21.0% in Eastern Kazakhstan to 33.9% in Mangystau oblast. Influenza infected persons aged 15-29 consisted 22.6% of the total infections, persons aged 30-64-10.7% and persons aged > 65 -1.7%.

Table 4. Age distribution of influenza and ARVI cases during the 2009-2010 epidemic in the territories of Kazakhstan
The percentage of hospitalized patients during the epidemic period from all influenza infected people averaged 2.9% throughout RK and fluctuated from 0.9% in Atyrau oblast to 7.5% in Almaty. The percentage of hospitalized patients from the whole population was 0.09%, and fluctuated from 0.02% in Atyrau and Aktobe oblasts to 0.2% and 0.4% in Almaty and Astana respectively. Cases with lethal outcome were registered in Eastern-Kazakhstan (5 cases) and Kostanay oblasts (1 case). The cause of the deaths was likely the delay in seeking to medical care. Among those lethal cases was one woman 38 weeks pregnant and a child aged 1 year.
During the virological study of patients in Kazakhstan during epidemic period 18 influenza viral strains were isolated and identified as influenza virus A1. Two of them were sent to St.-Petersburg to Research Institute of Influenza. According to the data of the RII laboratory of influenza evolutionary variance of Research Institute of Influenza these viruses A/Astana/818/09 and A/Astana/830/09 reacted only with antisera derived from the pandemic viral strain A/California/07/09 (H1N1). Consequently they belong to this subtype.
According to PCR-RT data in influenza and ARVI etiology agents of non-influenza ethiology increased After outbreak.
-
The 2009 influenza A (H1N1) epidemic in Kazakhstan began 3 weeks later (from 16thof till 22nd of October) than the epidemic in Russia (from 21st to 27thSeptember) [2, 3]. The epidemic in Kazakhstan started in the North-Eastern territories of the country at the border of Siberia and Ural and spread along a western and southern direction as observed in Russia [1, 5, 7-9].
The influenza epidemic in Kazakhstan was induced by a pandemic influenza virus similar to the strain A/California/07/09(H1N1) with a moderate intensity. According to mapping data of well-known pathogeni city sites this strain has a row of genetic irregularities which related it to mildly pathogenic viruses of 3rd group [4].
The epidemic intensity varied in different territories of Kazakhstan the as was observed in various regions of Russia. In Astana and in other north-eastern territories the epidemic intensity was longer duration (8-10 weeks) and and had higher morbidity levels (7.8%, 5.4% and 4.7%) compared to Zhambyl and Mangystau oblasts (duration for 4 weeks, morbidity 0.9-1.4%) situated in the South and south-western Kazakhstan (Fig. 1, 2). In Russia, in Siberia and Ural, the epidemic duration (7-8 and 7-5 weeks) and morbidity level (10.2% and 9.6%) were higher than similar parameters in the South and Privolzhskiy regions (5.8 and 5.7% weeks). Hence, epidemic intensity for appropriate boundary territories of Kazakhstan and Russia was in definite dependence. Morbidity level throughout regions of Russia, presented in the Figure 2, is higher than throughout territories of Kazakhstan, as the Federal Center initially conducts influenza sampling in urban territories where morbidity levels are higher than in rural areas.
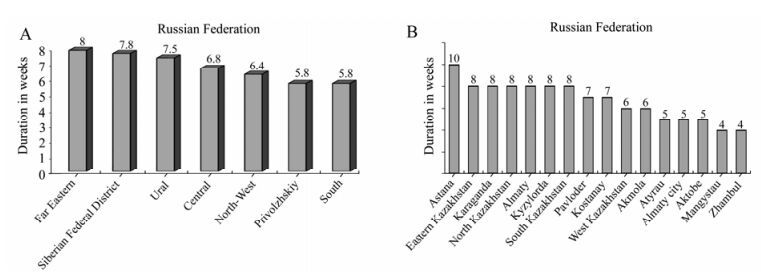
Figure 1. Duration of A(H1N1) 2009 epidemic in weeks in (A) Russian Federation and (B) Republic of Kazakhstan.
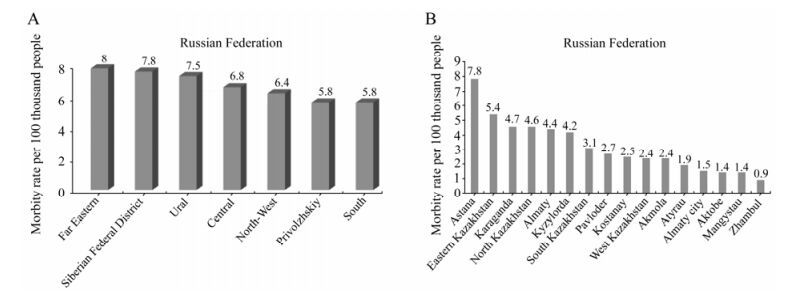
Figure 2. Influenza and ARVI morbidity A(H1N1)2009 in Russian Federation(A) and Republic of Kazakhstan(B).
The influenza and ARVI infection rates for children aged < 14 (65.0% compared to 52.4%) in Kazakhstan was higher in comparison with Russia. This can be understood in terms of differences in population demographics; the percentage of children in the population Kazakhstan is almost twice as many Russia children (24.2% compared to 13.0%) (Fig. 3). The role of people older than 65 in the epidemic was less significant and approximately equal (1.7%~1.9%).
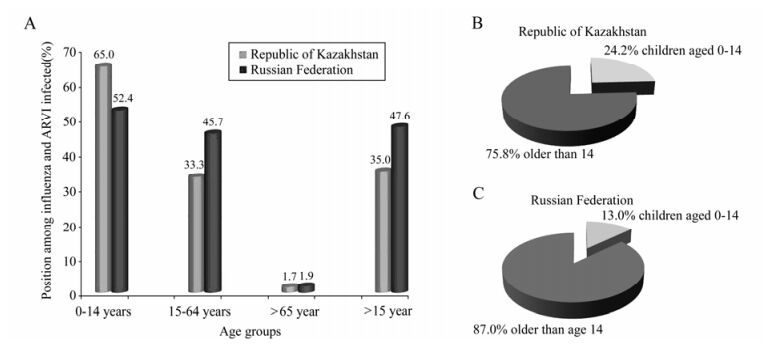
Figure 3. A: Age structure of cases infected with influenza and ARVI A(H1N1), 2009 people in the Republic of Kazakhstan and in 49 cities of Russian Federation. Percentage of cases in children aged < 14 years in Republic of Kazakhstan(B) and Russian Federation(C).
During the epidemic, the frequency of hospitalizetion from the whole population was 0.1% in Kazakhstan and 0.2% in Russia and the percentage of diseased people with influenza and ARVI was almost the same (2.9% against 2.6%).
Lethality from confirmed influenza cases in 49 cities of Russia was 3.2% which was approximately equal to the percentage of lethal outcomes in foreign countries (as determined from data collected by the WHO[10]).
Of the influenza mortalities recorded in Russia during this epidemic, 78.8% were adults aged 18-53, and persons > 65 -2.4%. Risk factors of influenza for lethal outcomes were chronic pathology and last period of pregnancy. Both in Kazakhstan and Russia the persons with lethal outcomes were either late seeking to medical care and or in the third trimester of pregnancy.
In conclusion, our analysis of epidemiological situation in two countries showed that epidemic in Kazakhstan was similar to epidemic in Russia with an unusually early beginning, evident monoaetiological character, involvement of all territories in the epidemic and the origin of the epidemic among the adult population. In this epidemic the high percentage of hospitalized and lethal outcomes influenza cases were registered. The percentage indicates heaviness of the influenza clinical tendency. Finally, differences in epidemic intensity in different territories of both countries and similarity of epidemiological process on boundary territories were also detected.













 DownLoad:
DownLoad: